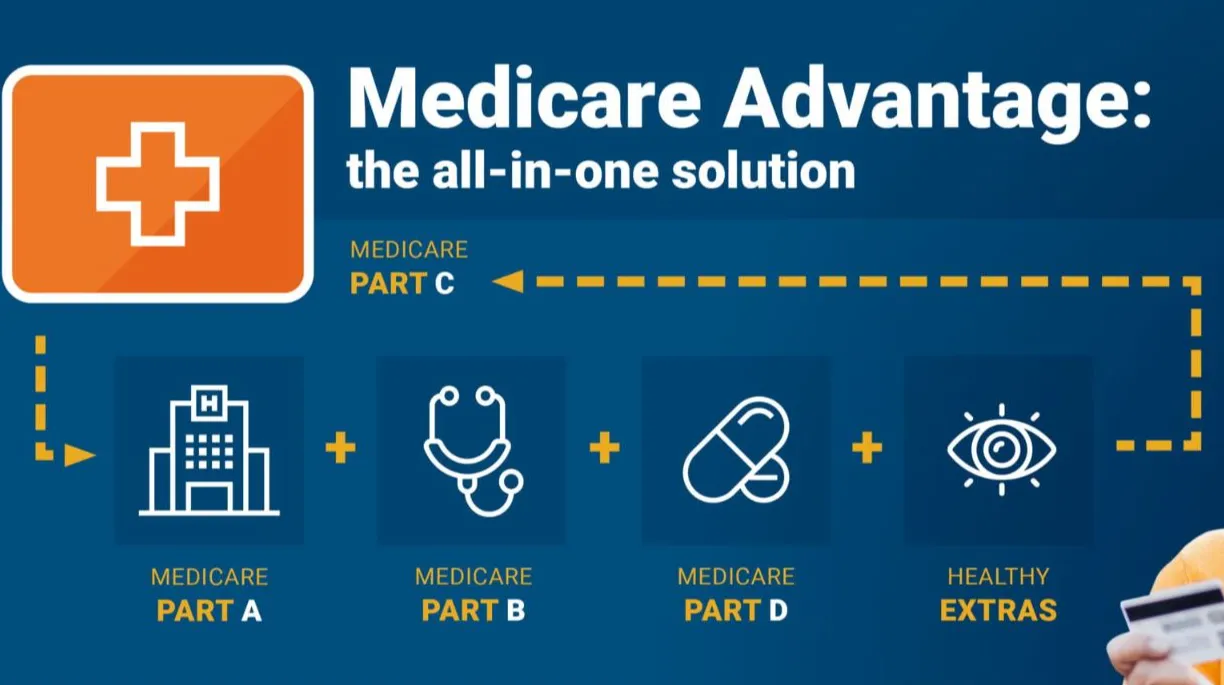
Medicare Advantage Enrollment Periods in California
Choosing the right time to enroll in or change your Medicare Advantage plan can save California residents money and prevent gaps in coverage. But Medicare doesn't let you switch plans whenever you want — there are specific enrollment windows throughout the year, each with its own rules. Understanding these periods is the first step toward making smarter decisions about your Medicare coverage in California.
The Annual Election Period (AEP): October 15 – December 7
The Annual Election Period — sometimes called the Annual Enrollment Period or Fall Open Enrollment — is the main window when California Medicare beneficiaries can make changes to their coverage. It runs every year from October 15 through December 7, and any changes you make take effect on January 1 of the following year.
During the AEP, California residents can:
- Switch from Original Medicare to a Medicare Advantage plan
- Switch from one type of Medicare Advantage plan to another
- Drop your Medicare Advantage plan and return to Original Medicare
- Join, switch, or drop a Medicare Part D prescription drug plan
This is the most important enrollment window of the year for California beneficiaries. Plan benefits, premiums, provider networks, and drug formularies change annually, so even if you're happy with your current plan, it's worth comparing your options every fall to make sure you're getting the best deal available in California.
Medicare Advantage Open Enrollment Period (MA OEP): January 1 – March 31
The Medicare Advantage Open Enrollment Period runs from January 1 through March 31 each year. This window is specifically for people who are already enrolled in a Medicare Advantage plan — it does not apply to California residents on Original Medicare.
During the MA OEP, you can:
- Switch to a different Medicare Advantage plan (with or without drug coverage)
- Drop your Medicare Advantage plan and return to Original Medicare (and optionally enroll in a stand-alone Part D plan)
You can only make one change during this period, and it takes effect the first of the month after the plan receives your enrollment request. This window is a safety net — if your California plan's benefits changed for the new year and you realize in January that it no longer meets your needs, the MA OEP gives you a second chance to make a move.
Special Enrollment Periods (SEPs)
Special Enrollment Periods allow California beneficiaries to make changes outside of the standard enrollment windows when you experience certain qualifying life events. Common triggers include:
- Moving to a new area — whether within California or to a different state — where your current plan isn't available
- Losing employer-sponsored coverage (retirement, job change, etc.)
- Qualifying for Medicaid or a Medicare Savings Program
- Your plan leaves your area or reduces its service area in California
- Living in an institution like a skilled nursing facility
SEPs vary in length depending on the qualifying event. For example, if you move within or out of California, you typically have two months to choose a new plan. If you're unsure whether you qualify for a SEP, contacting Medicare directly at 1-800-MEDICARE or talking to a licensed California agent can help clarify your options.
Initial Enrollment Period (IEP): When You First Become Eligible
If you're turning 65 or becoming eligible for Medicare due to a disability, your Initial Enrollment Period is a 7-month window centered around your 65th birthday month (or 25th month of disability benefits). It starts 3 months before your eligibility month, includes the eligibility month itself, and extends 3 months after.
During your IEP, you can enroll in Medicare, choose a Medicare Advantage plan, and/or pick a Part D drug plan. Enrolling during this window ensures you avoid late enrollment penalties and gaps in coverage. California residents should be aware that Medicare Advantage eligibility requires enrollment in both Medicare Part A and Part B first.
Key Dates at a Glance
Enroll, switch, or drop any Medicare plan
Switch MA plans or return to Original Medicare
7-month window around your 65th birthday
Triggered by qualifying life events
What Changed for 2026
Medicare Advantage continues to grow — for 2026, over 99% of Medicare beneficiaries have access to at least one Medicare Advantage plan, with an average of 39 plans available per beneficiary (KFF). For California residents, notable changes include:
- New $2,100 Part D out-of-pocket cap — the Inflation Reduction Act caps annual prescription drug spending, which affects Medicare Advantage plans that include drug coverage
- Lower average Part D premiums — stand-alone Part D premiums dropped from $38.31/month to $34.50/month nationally
- Plan benefit shifts — some California plans are adjusting supplemental benefits (dental, vision, hearing, fitness) so your current plan's extras may look different
These changes make it especially important to review your Annual Notice of Change (ANOC) when it arrives in September and separate fact from fiction when comparing plans during the AEP. For a comprehensive look at the latest enrollment windows, see Medicare Open Enrollment 2026. California residents should also stay informed about upcoming changes to Medicare that may affect plan availability and costs.
Tips for California Residents During Enrollment Periods
- Don't auto-renew without checking. Your plan changes every year. What worked last year might cost more or cover less in 2026.
- Use Medicare Plan Finder. Medicare.gov/plan-compare lets you compare plans by your California zip code, including premiums, copays, drug coverage, and star ratings.
- Check your doctors and drugs. Make sure your preferred California providers are still in-network and your medications are on the plan's formulary.
- Consider total cost, not just premiums. A $0 premium plan might have higher copays and deductibles. Use a financial checklist to compare apples to apples. Understanding the full breakdown of Medicare costs helps you plan your budget for the year.
- Know the common mistakes first-time enrollees make. Rushing through enrollment or picking a plan based on premium alone can cost you in the long run.
- Talk to a licensed California Medicare agent. A local agent can help you navigate your options at no cost to you — and they know which plans perform best in your area of California.